Avascular Necrosis (AVN): Symptoms, Causes & Best Treatment Options in Pune
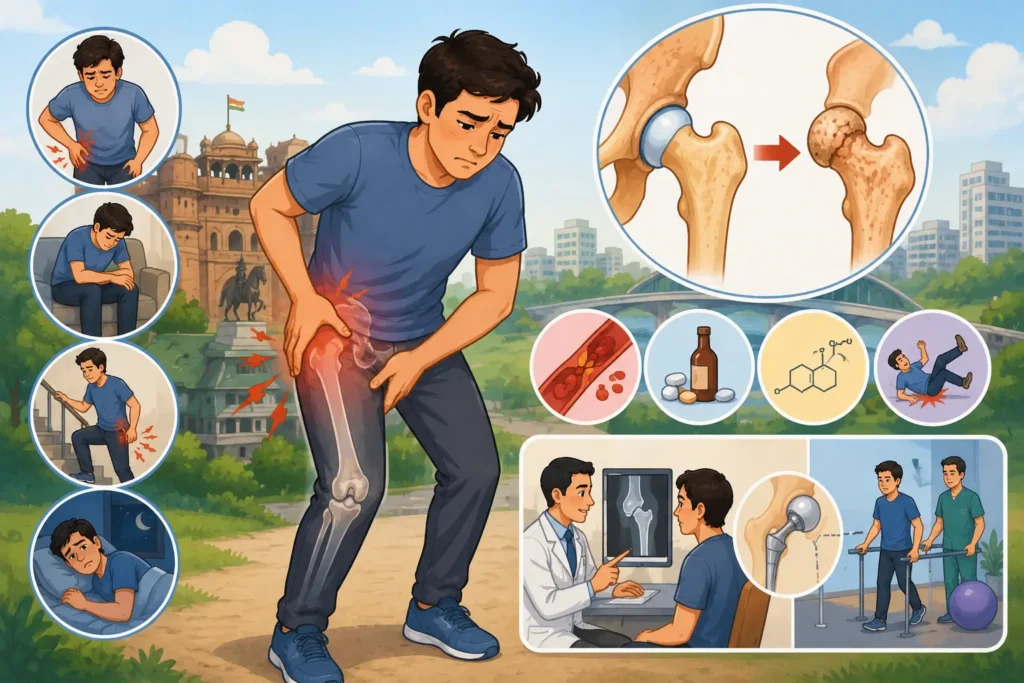
Persistent joint pain that does not improve with rest should never be ignored—especially when it affects your hip, knee, or shoulder. Many people assume it is just muscle pain, arthritis, or age-related discomfort, but sometimes the real cause is something more serious called Avascular Necrosis (AVN). AVN is a condition where the blood supply to the bone gets reduced or blocked, causing bone tissue to die gradually. If not treated early, it can lead to severe joint damage and may even require joint replacement surgery. The good news is that early diagnosis and timely treatment can help preserve the joint and prevent major surgery. At Dr. Vinayak Ghanate’s clinic in Baner, Pune, patients receive advanced orthopedic care for AVN, joint preservation, hip pain, trauma, sports injuries, and complex orthopedic reconstruction. What is Avascular Necrosis (AVN)? Avascular Necrosis, also known as Osteonecrosis, is a condition where the blood flow to a bone is interrupted. Without proper blood supply, the bone tissue starts dying, leading to: AVN most commonly affects: The hip is the most frequently affected joint, especially in adults between 30 and 50 years of age. Early Symptoms of AVN In the early stages, AVN may not cause obvious symptoms, which is why many patients ignore it. As the condition progresses, common symptoms include: 1. Deep Joint Pain Pain usually starts deep inside the joint, especially in the hip or groin area. Patients often describe it as: 2. Hip Pain While Walking If the hip is affected, pain may spread to: Many people think it is simple muscle pain and delay treatment. 3. Reduced Range of Motion You may notice: This happens as the joint surface becomes damaged. 4. Limping While Walking As pain worsens, patients often start limping to reduce pressure on the affected side. This is a strong sign that specialist evaluation is needed. 5. Pain Even During Rest In advanced AVN, pain may continue even while: This indicates progression of bone damage. Common Causes of Avascular Necrosis Several factors can reduce blood supply to the bone. 1. Long-Term Steroid Use Prolonged use of corticosteroids is one of the most common causes of AVN. This may happen in patients treated for: 2. Alcohol Consumption Heavy alcohol intake can affect fat metabolism and blood circulation, reducing blood supply to bones. 3. Trauma or Injury Fractures, hip dislocation, or severe injuries can damage the blood vessels supplying the bone. This is called post-traumatic AVN. 4. Medical Conditions Certain diseases increase AVN risk: 5. Unknown Causes In some patients, AVN develops without any clear reason. This is called idiopathic AVN. When Should You See an Orthopedic Surgeon? You should consult an orthopedic specialist if: Early diagnosis is the best way to avoid joint collapse. How AVN is Diagnosed At Dr. Vinayak Ghanate’s clinic, diagnosis begins with a detailed orthopedic evaluation. Further tests may include: MRI is often the best test to diagnose AVN in its earliest stage. Best Treatment Options for AVN in Pune Treatment depends on how early the condition is diagnosed. Non-Surgical Treatment (Early Stages) If AVN is detected early, joint preservation may be possible through: Early treatment can delay or even prevent joint replacement. Surgical Treatment (Advanced Stages) If the bone has already collapsed, surgery may be required. Treatment options include: The right approach depends on the stage of AVN. Why Choose Dr. Vinayak Ghanate for AVN Treatment in Pune? Dr. Vinayak Ghanate is known for advanced orthopedic care and precision-driven treatment planning. His expertise includes: His international training includes: Patients trust him for his honest consultation, precise diagnosis, and personalized treatment approach. Can AVN Be Cured Without Surgery? Yes, if diagnosed early. In Stage 1 or Stage 2 AVN, non-surgical or joint-preserving procedures can often prevent progression. But once the joint surface collapses, surgery usually becomes necessary. This is why early consultation is extremely important. Final Thoughts Avascular Necrosis is a serious condition, but it does not always mean immediate surgery. The earlier it is diagnosed, the better the chances of saving the joint. If you are experiencing unexplained hip pain, limping, groin pain, or difficulty walking, do not delay specialist evaluation. Timely treatment can protect your mobility, independence, and quality of life. Book Your Consultation in Pune If you are looking for the best AVN treatment in Pune, expert diagnosis for hip pain, or advanced orthopedic care for avascular necrosis, consult Dr. Vinayak Ghanate today. Take the first step toward pain-free movement and better joint health.